$9.4B For 'Innovative' Health Care Construction Forecasted for New York City
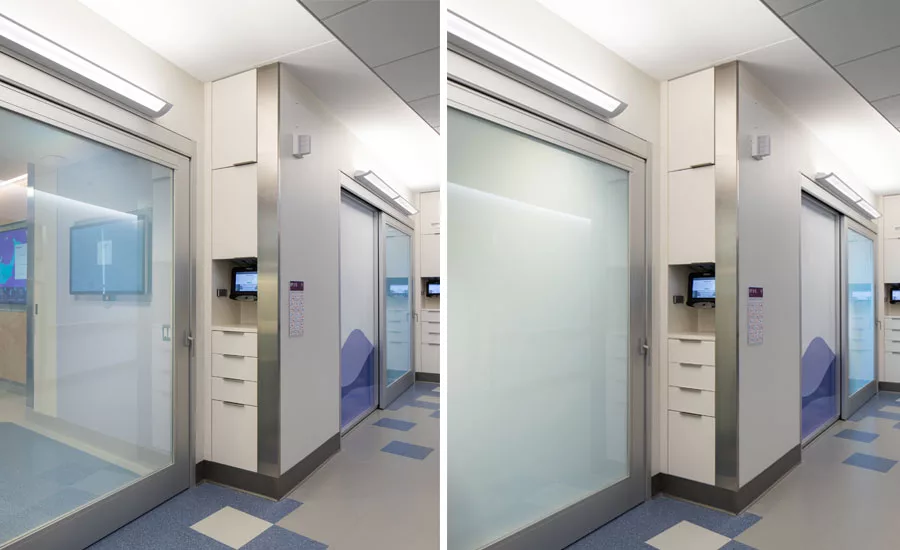
Intensive care rooms at NYU Langone's Helen L. and Martin S. Kimmel Pavilion have e-glass that can be made opaque (right) for privacy or kept clear (left) so that health care workers can monitor an infectious patient without having to constantly enter the room. PHOTO COURTESY NYU LANGONE
Modular components, flexible space and broader use of advanced filtration are some of the major trends in health care facilities construction in New York City, where the COVID-19 emergency offered a significant proof of concept.
That could mean a large volume of work ahead using innovative practices. From 2020 through 2023, total construction spending will increase by 38% over the prior 4-year period to $9.4 billion, according to a New York Building Congress forecast in a July 20 report. The assessment, called “NYC Checkup: An Examination of Healthcare & Life Sciences Construction,” notes the rapid renovations of existing facilities in the first half of this year “to handle an influx of infected patients.” Authored by the Building Congress —with contributions by the congress' Healthcare and Life Sciences Committee, Nancy J. Kelley & Associates, New York City Economic Development Corporation, Partnership Fund for New York City, Urbanomics and Dodge Data & Analytics—the report anticipates "spending will increase as hospitals and healthcare providers adapt to the next normal and prepare for a potential resurgence of COVID-19.”
Two important parts of that readiness—along with readiness for other healthcare needs—are upgrading air filtration systems and creating patient rooms that can be adjusted for pandemics, increased acute care needs and more.
Improved air supply
Paul Schwabacher, senior vice president of facilities management for NYU Langone, says one of the biggest trends will be "buildings that are adaptable and flexible.” For example, he notes that at the $1.4 billion, 830,000-square-foot Helen L. and Martin S. Kimmel Pavilion—recipient of ENR's New York regional and national Best Project awards for health care—patient “rooms had flexibility to operate at ICU level of care, so we could rapidly flex up, which is what we ended up doing for COVID-19.” At peak, the hospital was at 105% capacity, Schwabacher says.
Every infection-isolation room at Kimmel has vestibules that protect hallways from contagious patients. E-glass turns opaque on demand for privacy, or can remain clear so that nurses and doctors can constantly view a patient without having to enter the room and expose themselves to contagion.
These kinds of rooms may become the norm, says Carlo Scissura, president and CEO of the Building Congress. “Moving forward, the primary considerations for healthcare facilities will be resiliency, scalability and flexibility,” he says. “COVID-19 will likely lead to the construction of more [rooms] with ICU capabilities and flexible patient capacity, such as larger medical gas connections, additional power and emergency power.”
The rooms at Kimmel are also equipped with negative-air-pressure controls to reroute infected air away from other patients and staff. Hospital-wide, HEPA systems filter air at the same high rate most hospitals only require for operating rooms—up to 12 air changes per hour in patient care areas. “Older buildings have much lower” change rates of less than half, Schwabacher says, except in their critical care areas.
Looking for quick answers on construction and engineering topics?
Try Ask ENR, our new smart AI search tool.
Ask ENR →
NYC Health + Hospitals, the municipal health care system with more than 70 facilities including 11 hospitals and five long-term care facilities, is planning to upgrade filtration and other sanitizing systems. The Building Congress’ report says the city allocated $931.6 million for NYC Health + Hospitals’ fiscal year 2021 capital budget. Over the next four years, the system has committed $3.2 billion in capital spending, with $1.1 billion expected in 2020.
“As we look to the future, we need to enhance our air quality systems,” Christine Flaherty, senior vice president in the office of facilities development, said in a July 7 online lecture for Columbia University’s Center for Buildings, Infrastructure and Public Space. “There is a definite need for long-term investment in increasing our air exchanges, further enhancing our systems with filtration, UV lighting, [and] having more controls on negative and positive air pressure capabilities in many of our areas.”
All this, Flaherty said, represents “approximately half a billion of dollars of need.”
Upgrading air filtration systems in existing buildings costs much more than building top level systems into the structures from the start, Schwabacher explains. “To retrofit would be incredibly expensive,” he says, because HEPA systems require more space for components like bigger fan motors, and air handlers.
Building in such systems up front costs more, he concedes, but it is “by no means 50% [higher]—it’s much less than that.” The pricier systems and features are demonstrating their payoff. “As the crisis in New York City has stabilized, healthcare institutions see the value in investing in preventative infrastructure, pandemic preparedness and new technologies,” Scissura says.
Modular saves money, increases quality
Another trend in health care construction in the city will help teams lower costs. Modular construction is being used to shorten build time, reduce construction costs and minimize disruption to active hospital operations, according to the Building Congress report.
“While a project’s superstructure is being erected, the mechanical space, building envelope and standardized elements, such as patient rooms, operating suites and bathrooms, can be simultaneously built offsite,” Craig Miller, healthcare practice leader at Jacobs is quoted in the report. “Significant cost saving advantages are realized due to the increased productivity, reduced material waste and lower safety risks.”
Group PMX LLC successfully used modular construction on several projects, including a 2,800-gross-sq-ft trauma center and a 2,500 gross-sq-ft mechanical equipment room, the report said.
To be sure, the city’s licensing and jurisdictional issues can limit modular construction methods. Multiple municipal agencies must approve the movement of prefabricated units on city streets, and construction sites must also have enough space to stage the modules before placing them on the superstructure.
But the benefits are clear when looking at the Kimmel Pavilion’s construction. Patient rooms’ bathroom pods with a toilet, sink, shower and bedpan washer—so pans don’t need be carried away—were prefabricated in New Jersey and installed before the fit out. It was an economical option that also “made it easier to go quickly,” Schwabacher says. Also, the prefabbed loos provide “better quality control and better consistency … so for long term maintenance it’s easier because they’re all the same.”
Flaherty said that during initial surge work in the midst of the pandemic, which ate up “millions of trades-workers' hours,” NYC Health + Hospitals “ didn’t find as many opportunities as we would’ve liked for prefab” because it was “just sourcing [materials] in the moment.” But she emphasized, it’s “definitely an area we do want to look at as opportunities to be more innovative.”
So, it seems, do all health facilities developers in the city. Scissura says, “Future-focused healthcare facilities are being reimagined around patient experience, operational efficiency and seamless integration of technology.”




